Fauci Admits the Concept of "Social Distancing" was not Based in Science
The concept of social distancing actually arose from a 15 Year old's science fair project.
During the recent Senate Select Subcommittee hearing Anthony Fauci acknowledged that the guidelines for six feet of separation, aka “social distancing”, to limit the spread of SARS-CoV-2 just “sort of appeared” without scientific input.
Fauci stated that he was not responsible for creating that rule and that it came from the CDC. He also admitted that the guideline was not based in science. Fauci said that what he meant was, “there wasn’t a controlled trial that said compare six feet with three feet with ten feet. So there wasn’t that scientific evaluation of it.”
The so-called “science” behind social distancing
Dr. Robert Glass’s daughter Laura, then 14, had done a class project in which she built a model of social networks at her Albuquerque high school, and when Dr. Glass looked at it, he was intrigued. The Albuquerque High sophomore’s research later became the basis for social distancing.
Source: https://www.abqjournal.com/1450579/social-distancing-born-in-abq-teens-science-project.html
Her project, based on computer simulations of human interaction, motivated research that resulted in the social distancing and self-isolation policies that were used to curtail the spread of SARS-CoV-2.
Laura, with some guidance from her dad, devised a computer simulation that showed how people – family members, co-workers, students in schools, people in social situations – interact. Based on her findings, her program showed that in a hypothetical town of 10,000 people, 5,000 would be infected during a pandemic if no measures were taken, but only 500 would be infected if the schools were closed. Her plan for slowing the spread of pandemics was simple, close the schools and keep the kids at home. Refined research suggested that with more intense infections closures might have to include workplaces and social situations.
The Centers for Disease Control and Prevention made social distancing – called Non-Pharmaceutical Interventions, or NPIs – official U.S. policy in February 2007.
There are many factors that contribute to spread of virus
‘Airborne transmission,’ comprising both droplet spray and aerosol modes, describes the direct inoculation of virus particles from the air into the respiratory tract without an intermediate. Airborne routes (droplet spray and aerosol) seemed to be more important in SARS coronavirus spread.
Factors that contribute to airborne transmission of viruses can be classified into three broad categories; 1. host factors 2. characteristics of the virus and 3. environmental factors.
Viral load of the emitter, duration of exposure, and susceptibility of an individual to infection are all important but there is an intimate interplay between these factors and environmental conditions. Key environmental factors involved in virus transmission include temperature, pH, relative humidity and ventilation to name a few.
Animal models have elucidated potential mechanisms by which humidity and temperature influence human influenza virus transmission. A significant decrease in transmission efficiency occurs with increasing relative humidity (RH) and during summer months. Lowen et al. showed in experiments in the guinea pig transmission model that at 20°C, transmission efficiency of an influenza A/H3N2 isolate displayed a bimodal dependence on RH, with airborne (i.e. droplet or aerosol) transmission being maximal at 20–35% RH, poor at 50% RH, moderate at 65% RH, and absent at 80% RH. Transmission was abolished at high temperature (30°C), regardless of RH. Therefore, both cold and dry conditions favor virus transmission.
The size of a droplet was thought to determine how far it will travel from the infected person. Authors of an editorial “Two metres or one: what is the evidence for physical distancing in covid-19?” published in BMJ stated, “Rules that stipulate a single specific physical distance between individuals to reduce transmission of SARS-CoV-2, the virus causing covid-19, are based on an outdated, dichotomous notion of respiratory droplet size.” The 1-2 m rule is based on a longstanding framework which dichotomizes respiratory droplets into two sizes, large and small. The framework simplistically suggests large droplets fall through the air more quickly than they evaporate and small droplets (later called aerosols or airborne droplets) evaporate more quickly than they fall.
“This overlooks the physics of respiratory emissions, where droplets of all sizes are trapped and moved by the exhaled moist and hot turbulent gas cloud that keeps them concentrated as it carries them over metres in a few seconds.” After the cloud slows sufficiently, ventilation, specific patterns of airflow, and type of activity become important.
Improving ventilation can help reduce virus particles in indoor spaces
There is strong and sufficient evidence to demonstrate the association between ventilation, air movements in buildings and the transmission/spread of infectious diseases such as measles, tuberculosis, chickenpox, influenza, smallpox and SARS.
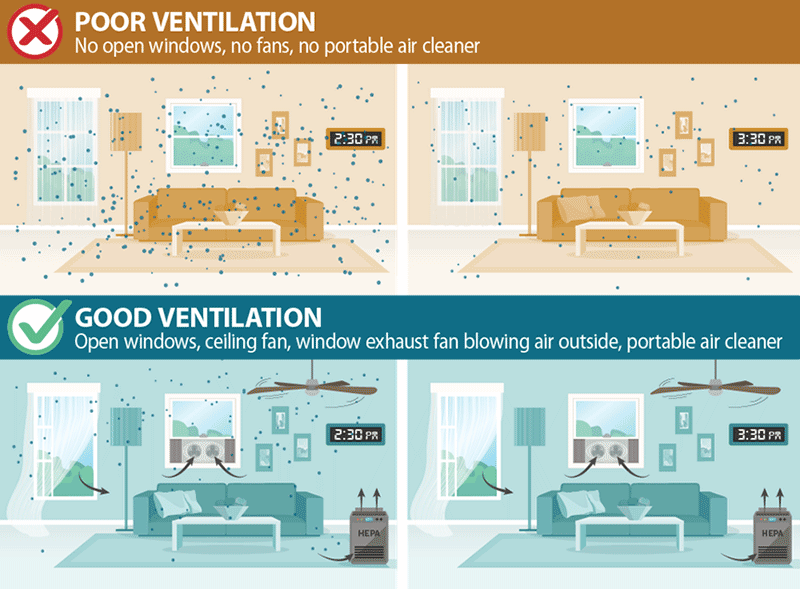
Even CDC finally recognized the importance of ventilation in reducing virus transmission. When we stay in a closed space viral contaminated particles will circulate in the closed room and anyone healthy can inhale it and get sick. However if we keep windows open and allow fresh air in, the viral load will be diluted and disperse thus one will inhale a lower load of virus laden droplets.
Source: https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/improving-ventilation-home.html
It wasn’t until April of last year that CDC recommended people ventilate their home by getting fresh air into their home, filtering the air that is there, and improving air flow.
There is more to just staying six feet away from people to decrease virus spread. All the environmental factors affect how far droplets spread and how long they will stay suspended in the air.
The best thing people could have done was to open their doors and windows and go outside. Influenza epidemics begin in the fall/winter partly as a result of people crowding indoors. These epidemics end in the spring time when the weather warms up, people open their windows and go outdoors.









It’s also completely crazy to think how they were closing off playgrounds and parks in CA when I was there. Literally they put up fences around them to keep kids away. And how many people were going outside jogging, walking, playing with masks on. Outside…
We reverted to medieval way of thinking. It might as well been the virus was a magic spell and we needed to recite something and turn around 6 times while throwing salt over our shoulder. And it isn’t as if we didn’t have decades of research with OTHER respiratory viruses and past pandemics. The plexiglass barriers and footstep tracks at the grocery store were my favorite. I thought about reorganizing the floor stickers to make some dance moves.
Great article. Thank you.
Wow. There's some information here that I was completely unaware of. A 14-year-old's science project?