Off Target or Non-specific Effects of Vaccines
Vaccines were not tested for their effects on overall health before being introduced
It is known that vaccines against infectious diseases have complex non-specific effects on morbidity and mortality that extend beyond prevention of the targeted disease.
When developing vaccines, researchers focus on the ability of the vaccine to protect against the disease for which it is being designed. Efficacy of a vaccine is a measure of how well the vaccine prevents the disease it was developed against.
CDC defines vaccine efficacy as:
Vaccine effectiveness is a measure of how well vaccination protects people against health outcomes such as infection, symptomatic illness, hospitalization, and death.
Vaccines have “non-specific effects”
Vaccines not only protect against the target infection; they also affect the susceptibility to other infections. These effects have been called the “non-specific effects” of vaccines.
The non-specific effects are found to vary depending on the type of vaccine being administered. Live vaccines have been associated with beneficial non-specific effects. Inactivated vaccines, although protecting against the vaccine-targeted infections, may possibly increase susceptibility to other infections.
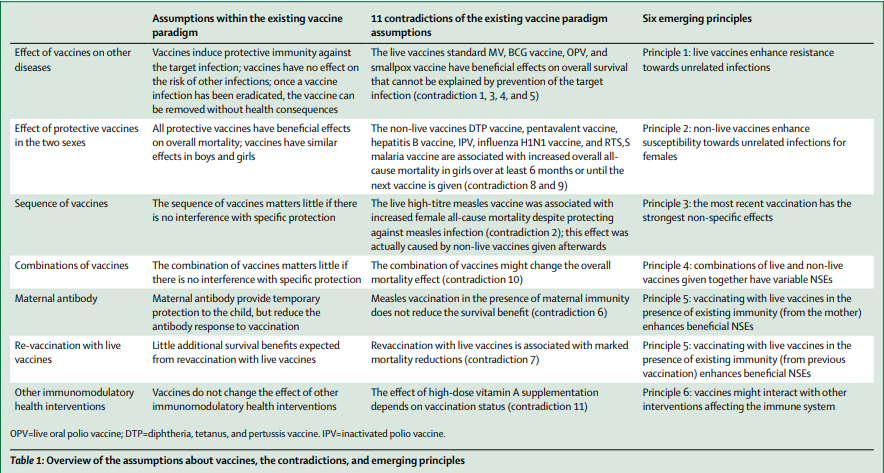
In this article, Dr. Christine Stabell Benn outlines six principles that explain emerging paradigms about non-specific effects of vaccines.
Source: https://sci-hub.ru/10.1016/S1473-3099(19)30742-X
Live vaccines enhance resistance towards unrelated infections.
Inactivated vaccines enhance the susceptibility of girls to unrelated infections. In addition, inactivated vaccines are associated with increased all-cause mortality specifically in females.
The most recently administered vaccination has the strongest non-specific effects.
Combinations of live and inactivated vaccines given together have variable non-specific health effects.
Vaccinating children with live vaccines in the presence of maternal immunity enhances beneficial non-specific effects and reduces mortality.
Finally, vaccines might interact with other co-administered health interventions, for example vitamin A supplementation.
Effects of vaccines on susceptibility to other infections
A study to compare vaccinated and unvaccinated children on a broad range of health outcomes found the vaccinated were significantly less likely than the unvaccinated to have been diagnosed with chickenpox and pertussis, but, contrary to expectation, were significantly more likely to have been diagnosed with otitis media, pneumonia, allergic rhinitis, eczema, diabetes, and neurodevelopmental disorders. The vaccinated were also more likely to have used antibiotics, allergy and fever medications; to have been fitted with ventilation ear tubes; visited a doctor for a health issue in the previous year, and been hospitalized.
A study by another group using children from three pediatric medical practices in the United States confirmed the results that vaccinated children were significantly more likely than unvaccinated children to be diagnosed with severe allergies, autism, gastrointestinal disorders, asthma, ADHD, and chronic ear infections. Results from their analysis of relationships between vaccination and breastfeeding status also showed that the lowest percentages of adverse diagnoses were observed for "unvaccinated and breastfed" children; the highest were observed for "vaccinated and not breastfed" children.
Beneficial effects of vaccines on mortality
There is a substantial body of evidence from randomized controlled trials (RCTs) that, until the next vaccine is given, Bacillus Calmette-Guerin (BCG) and measles vaccines (both live attenuated vaccines) have potent beneficial nonspecific effects.
Studies have observed that BCG vaccine approximately halves mortality from infections other than tuberculosis; provided vitamin A was not given at birth and measles vaccine approximately halves mortality from infections other than measles; this effect may be stronger if the child still has maternal antibody.
A study of infants in Guinea-Bissau, West Africa published in the BMJ found:
After cluster, age, and other vaccines were adjusted for, BCG was associated with significantly lower mortality (0.55 (0.36 to 0.85)). However, recipients of one dose of diphtheria, tetanus, and pertussis or polio vaccines had higher mortality than children who had received none of these vaccines (1.84 (1.10 to 3.10) for diphtheria, tetanus, and pertussis). Recipients of measles vaccine had a mortality ratio of 0.48 (0.27 to 0.87). When deaths from measles were excluded from the analysis the mortality ratio was 0.51 (0.28 to 0.95).
Measles vaccine may be one of the truly important childhood vaccines. Complications of measles infection include pneumonia, encephalitis and death. One of the most unique—and most dangerous—features of measles pathogenesis is its ability to reset the immune systems of infected patients. During the acute phase of infection, measles induces immune suppression through a process called immune amnesia. This means measles virus depletes a persons antibody repertoires, partially obliterating immune memory to most previously encountered pathogens.
Timing of administration of measles vaccine has been shown to be important. The current age of measles vaccination is typically between 9 months and 15 months of age to avoid vaccinating in the presence of maternal measles antibody that might reduce measles-specific antibody response. However, the beneficial effect of measles vaccine on survival is stronger when it is given before the child was 12 months old. One study found measles vaccine in the presence of maternal antibodies was consistently associated with lower mortality compared with measles vaccine in the absence of maternal antibodies, the combined meta-estimate indicating 55% (35-68%) lower mortality. In fact, the relative change in all cause mortality between 4–5 months and 5 years was reduced 78% (95% CI 36–93%) in children who received an early measles vaccine dose in the presence versus in the absence of maternal measles antibody. Even though there is a beneficial effect for both boys and girls, the effects of live attenuated vaccines on all cause mortality are higher among girls than boys.
On the other hand, whole-cell diphtheria-tetanus-pertussis (DTP) vaccine increases mortality from infections other than diphtheria, tetanus, and pertussis and this effect is stronger in girls than boys with increased overall mortality for girls. In a combined analysis of 17 studies, girls have 1·47 (1·18–1·84) higher mortality than boys after receiving the DTP vaccine. Similarly, administration of IPV, a hepatitis B vaccine, a pentavalent (DTP, hepatitis B vaccine, and Haemophilus influenzae b) vaccine, and the H1N1 influenza vaccine have been associated with higher mortality in girls than in boys for reasons are not well understood yet.
Keep in mind tuberculosis, polio, diphtheria, tetanus, pertussis, and measles, are not the leading causes of death in children, even in nonimmunized communities.
These paradigms extend to COVID genetic vaccines
Dr. Stabell Benn analyzed the effects of the COVID genetic vaccines with respect to impact on overall mortality.
She found the two types of vaccines differed significantly with respect to impact on overall mortality (p=0.030) as well as non-accident, non-COVID-19 deaths (p=0.046).
The adenovirus-vector vaccines were associated with protection against COVID-19 deaths (RR=0.11 (0.02-0.87)) and non-accident, non-COVID-19 deaths (RR=0.38 (0.17-0.88)).
Even though the adenovirus-vector is replication deficient, it may prime the immune system in a way similar to a “live” vaccine. However, governments chose to favor the mRNA injections over the adenovirus vectored genetic vaccines.
Dr. Benn concluded:
Ironically, the rich countries in Europe and USA have emphasized the more expensive mRNA vaccines because these vaccines have slightly better short-term vaccine efficacy against COVID19 than the relatively inexpensive adenovirus-vector vaccines, and due to the detection of a rare blood clotting disorder associated with the adenovirus-vector vaccines. While this decision is understandable in the short-term during a situation with high COVID-19-related mortality, in the endemic situation in which COVID-19-related deaths have decreased this decision may need to be reassessed. Otherwise, if the protective effects of adenovirus-vector vaccines on overall mortality in the RCTs reflect the reality, this could turn out to be a very costly decision, both economically and health wise.
It would be interesting to have an update on this study now over one year after it was first released.
It is time to modify the routine vaccination schedule
Under the currently recommended pediatric vaccination schedule, U.S. children receive up to 48 doses of vaccines for 14 diseases from birth to age six years, a figure that has steadily increased since the 1950s. Now, children could receive as many as 27 shots by 2 years of age and up to six shots in a single visit.
Given there are some beneficial nonspecific effects of live attenuated vaccines, we shouldn’t throw the baby out with the bathwater. However, it is time to rethink the vaccination schedule for children given these emerging paradigms about the non-specific effects of vaccines.